Assessments

Patient-Reported Outcomes
In addition to strictly biological markers of chronic post-surgical pain, A2CPS also considers markers across psychosocial and clinical domains. That includes patient questionnaires, which assess aspects of pain, medication use, disability and function, fatigue, sleep, activity levels, depression, anxiety, and social support. We also use tests that measure patients' functional abilities, such as how long it takes to walk ten meters, or to sit down and stand up from a chair five times in a row.
Functional Testing
A2CPS assesses pain with movement using functional testing. Participants with knee replacement surgery perform two tests: a 10 meter walk and a 5 times sit-to-stand test. Participants with thoracic surgery do a deep breathing “task” and a coughing “task.” These are called functional testing, but our primary interest is how much pain is caused by the movements rather than performance on the tests.
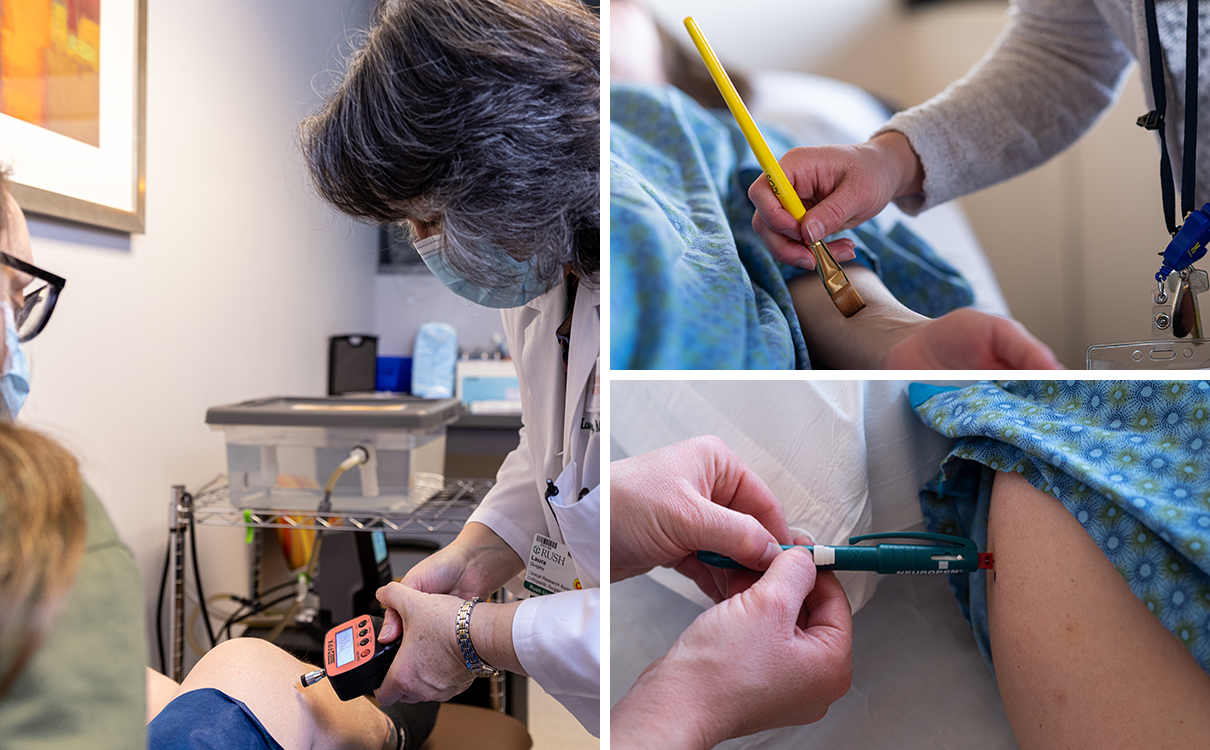
Quantitative Sensory Testing (QST)
Pain is inherently a subjective experience that arises from complex activity throughout the nervous system. Within the central nervous system (CNS), pain modulation mechanisms can amplify or dampen incoming signals from the periphery, shifting the brain's perception of pain. In people with chronic pain, the balance may be tipped toward pain amplification. Studies in animals have allowed us to better understand these modulation mechanisms, but these types of invasive studies are not possible in humans.
Instead, we use a type of indirect measure, called quantitative sensory testing (QST), that provides a window into what might be happening in the nervous system. For example, we measure pressure pain thresholds (PPTs) at both the site of pain (surgery) and at a distant site. Increased sensitivity at the surgical site may arise from local (peripheral) and/or central modulation mechanisms, whereas increased sensitivity at a distant site - or more widespread pain in general - suggests the involvement of CNS-mediated pain modulation.
The repeated Neuropen probe test allows us to assess what is called "temporal summation" of pain. The stimulus intensity remains the same over time, so when individuals rate the pain as increasing, that indirectly indicates that the CNS is amplifying incoming pain signals. Although temporal summation is a common response to painful stimuli, it might suggest someone has an increased risk, or vulnerability, for the CNS to amplify peripheral pain signals.
Conversely, we use the conditioned pain modulation (CPM) assessment to indirectly measure inhibitory pain modulation. According to this "pain inhibits pain" phenomenon, the response to a painful stimulus is normally reduced when it is presented together with another pain stimulus presented elsewhere on the body - in our case, the cold-water immersion bath. In people who do not experience this decrease compared to the initial stimulus, it may signal a loss of endogenous pain inhibition, leading to heightened pain processing. These are just three examples of the many processes involved in pain modulation, but these QST measures may serve as biomarkers or indicators for the transition to chronic pain.
