Brain Imaging
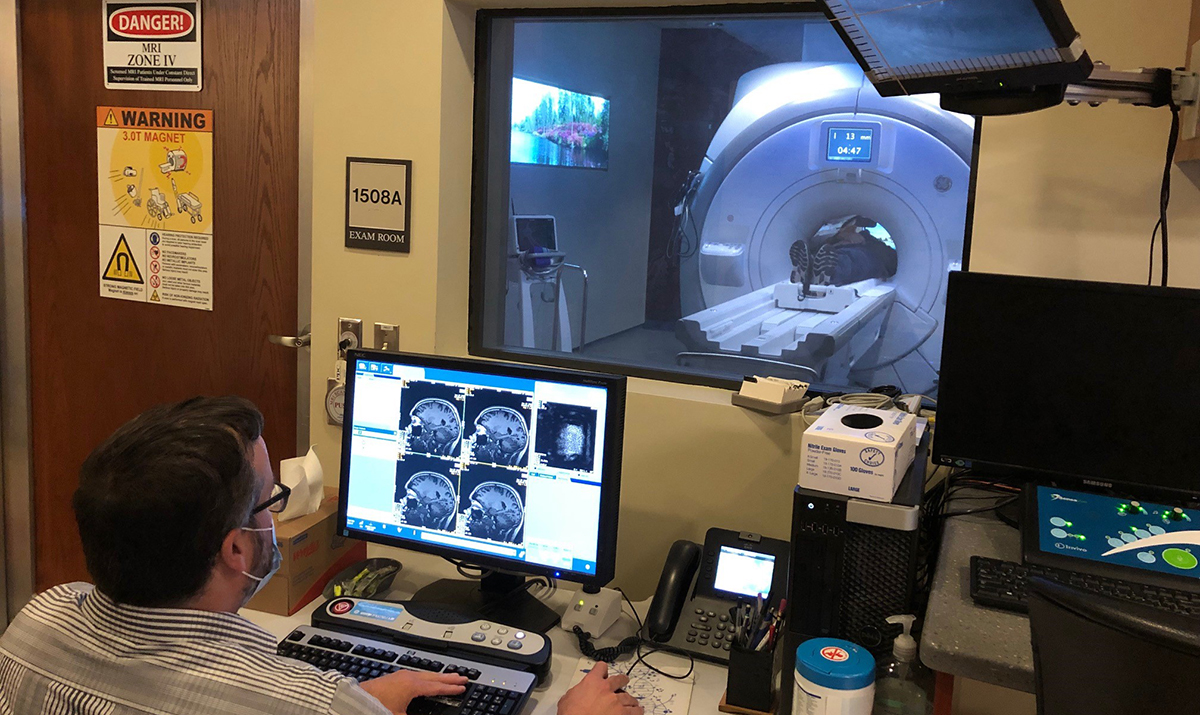
Brain imaging with magnetic resonance imaging (MRI) presents a major barrier to enrolling participants in the A2CPS study, but we do it because of the tremendous power that the technique adds to our data. The major aim of A2CPS is to identify biomarkers or biosignatures that can help diagnose, predict, treat and even prevent chronic post-surgical pain. Neuroimaging provides some of the most powerful and non-invasive biomarkers of the risk for chronic pain.
In 2013, A2CPS investigators Tor Wager and Martin Lindquist published a landmark paper showing a "pain signature" detected with MRI. Using machine learning analysis, they identified activity across the brain in healthy people during heat-induced pain. The signature includes regions known to be involved in pain processing: the thalamus, insula, anterior cingulate cortex, and periaqueductal gray, among others.
In another important study also published in 2013, A. Vania Apkarian showed that brain signatures measured with MRI could actually predict among those with acute back pain who would go on to develop chronic pain and those whose pain resolved. They found that the transition to chronic pain involved a switch from pain processing mainly in sensory-discriminatory areas that detect physical pain to brain areas more involved with emotional processing and assigning meaning to pain.
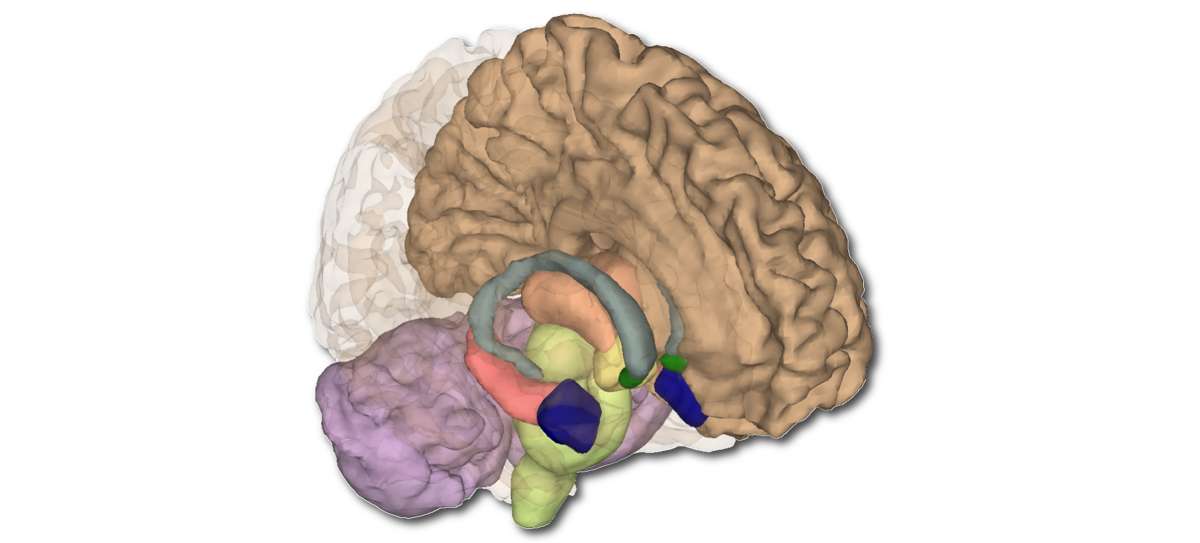
These studies are among the many that have guided A2CPS when it comes to neuroimaging. Our selected biomarkers are derived from high-resolution anatomic (structural) images that reveal brain morphology, diffusion MRI to infer structural connectivity; and functional MRI (fMRI) that provides insight into functional connectivity.